You may fall down. Your foot feels floppy and difficult to control.
So what should you do?
1. Use a cold compress for about 5 minutes over the back of the leg to limit inflammation, or rub an ice cube around the area for a few seconds at a time.
2. It’s best if you don’t put weight through the leg. If you can’t be carried or stretchered away, use crutches or lean on someone’s shoulders and hop. If you have to put the foot down, turn your foot out sideways, and try to keep your weight on the heel.
The damage
The tendon can break completely, creating a loss of continuity in its structure, or it may be partly torn, so that some strands are still joined up. A tear can happen in any part of the tendon’s length. The broken ends may stay close together, technically in apposition, or they may be widely separated, leaving a visible defect or gap of several inches in the back of the lower leg.
Who gets this injury?
Young adults, both males and females, are most likely to be victims of Achilles rupture. Among older people, the tear can happen relatively easily if the tendon has been weakened through injury, illness and especially previous injection. Achilles tendon rupture is uncommon in young teenagers, and extremely rare in pre-adolescent children.
It can happen during walking or running, but it’s most common through explosive sports which involve changing direction at speed, such as squash, badminton, soccer, American football and rugby.
Reasons underlying Achilles tendon rupture:
The injury appears to happen out of the blue, but there’s usually a reason for it, or sometimes a combination of several causes. Tightness and weakness in the calf muscles are major factors.
Dehydration
If you don’t drink enough water, you increase your risk of injury to the calf muscles and Achilles tendons. Cramp in the calf muscles is a common result of dehydration, and it can cause tightness. Dehydration is one of the main reasons why Achilles tendon rupture happens well into a bout of explosive exercise such as a game of squash or badminton, and not at the beginning when the body has not warmed up yet.
Muscle imbalance and overload
If the calf musculature is relatively tight or weak, it is more likely to give way if you stretch or stress it too hard.
Tightness can be caused by a variety of factors, including lack of stretching and slow circulation. Women who habitually wear high-heeled shoes cause significant shortening in their calves, especially if they are also inactive and sit or stand still for long periods. In both men and women, the calf musculature may be tight through compensating for weakness in the hamstrings. The muscles of the dominant leg may be tight because they’re used more heavily.
Weakness can be a factor. Your non-dominant leg may be significantly weak relative to the other leg, just through the way you move. Previous injuries to the knee or calf muscles can make you vulnerable to Achilles tendon tear, if you haven’t recovered fully. Inadequately rehabilitated injuries in other parts of the legs may leave a residue of imbalance, with a risk of overload of the calf and Achilles tendon.
In particular, weakness in the soleus muscle plays an important part in Achilles tendon rupture, because of the muscle’s relationship to the tendon, and its role in the leg’s blood flow.
Circulatory deficiency
A reduction of the blood flow through the feet and legs, however slight, can compromise the efficiency of the calf muscles and Achilles tendons.
In women, hormonal changes, for instance pre-menstrually, in the early stages of the period, or during pregnancy, can lead to cramps or sluggish blood flow in the lower legs.
In both men and women, cold weather conditions, inactivity and varicose veins can slow down the circulation in the calf musculature.
Conditions such as intermittent claudication and diabetes, which affect the leg circulation, can contribute to Achilles tendon rupture.
Any drugs which affect the circulatory system can be a background factor in Achilles tendon rupture.
Fatigue
Tiredness is another reason why the rupture often happens well into a walk, run, game or training session. It may be physical, mental, emotional, or a combination of all three. A busy lifestyle, lack of fitness or insufficient preparation for strenuous, explosive exercise can all contribute. Weakness because of previous injuries can cause localized fatigue in the calf muscles.
Injections
Injections into the central core of the Achilles tendon are known to weaken the tendon substance and give rise to the risk of subsequent tendon rupture. The tear may happen several weeks after an injection has been administered.
Drugs
Certain drugs, such as steroids, are known to weaken tendons and therefore expose them to an increased risk of tearing. Fluoroquinolones are antibiotics which are known to have damaging effects on tendons, muscles, joints, nerves and the central nervous system (U.S. Food and Drugs Administration ()FDA) updated warning, 2016). Achilles tendon rupture is a specific risk of these antibiotics, and the FDA issued its highest level warning of this in 2008.
Shoes
Shoes affect the foot and leg mechanics during walking, running and jumping. If there is not enough cushioning under the heel, impact from walking, running or jumping can cause jarring stresses which the Achilles tendon cannot absorb fully. If the heel counter of the shoe is unstable, the heel rolls excessively from side to side, causing adverse tension in the Achilles tendon.

If there is direct pressure from the back of the shoe or boot against the Achilles tendon, there is a risk not only of friction irritation leading to Achilles tendon pain, but also of mechanical impediment, as the intruding shoe-back prevents the tendon from shortening and lengthening freely.


Diagnosis
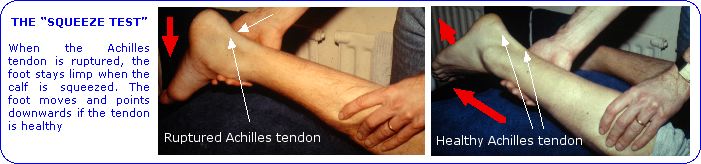
The injury is easy to diagnose, because it is so dramatic, and the site of pain is well defined. The Simmonds test, also known as the "squeeze test", is the simplest way to confirm the rupture. You lie on the couch, the practitioner supports your foot while you turn over to lie prone (on your stomach). Then, if the practitioner lets go of your foot, you can’t control it and it drops, forming a right angle at the ankle. Having let the foot drop, the practitioner squeezes the calf muscles gently, which is painless. The test is positive if the foot does not respond by pointing away from the body. If there is any doubt, for instance if there might be a partial rather than a total tear, or if there is a special reason for establishing a definitive diagnosis, a scan may be done.
Treatment options
Following even total rupture, the Achilles tendon is capable of mending naturally. Many years ago, Craig Sharp, the expert sports scientist who headed the pioneering British Olympic Medical Centre, told me that physiologists were well aware that tendons could mend themselves, "it's only medics who believe this is not true for human tendons". Craig's guidance was invaluable in helping me develop new rehabilitation options for Achilles tendon injuries.
The treatment options are the same for partial or total rupture of the Achilles tendon. The priority in treatment is to ensure that the tendon is not allowed to lengthen out as the result of the rupture. If it does, the tendon will become functionally inefficient: the patient will be unable to push off the ball of the foot efficiently when walking, running or jumping. Unwanted lengthening will happen if the tendon is not protected and held at its normal functional length during the initial healing period until the calf musculature has regained adequate strength and coordination.
There are three main options for treating the ruptured Achilles tendon. Often patients are only offered a choice between two, the traditional conservative treatment of putting the leg into plaster-of-Paris, or an operation to stitch the broken ends of the tendon together. The third, but less well-known option is active rehabilitation from the earliest stage possible, using a removable cast or adjustable walking boot to protect the tendon at the correct length.
Whatever treatment option you choose, you must take care of the circulation in your leg at all times; avoid any drugs or medicines which might be harmful; and eat a healthy, balanced diet, including plenty of fresh, preferably organic vegetables.
Active rehabilitation treatment
Active non-surgical treatment for the ruptured Achilles tendon is based on several principles: 1) the tendon canmend naturally and early activity helps functional recovery; 2) the torn Achilles tendon has to be protected from lengthening out as it recovers; 3) exercise activities for the rest of the body can be carried out safely; 4) the recovery process can be monitored at every stage; 5) there is less risk of complications such as Sudeck's condition.
Treatment can start immediately after the injury has happened. The leg is protected in a removable adjustable cast or walking boot, and is usually taped to hold the foot securely pointing downwards in the correct position during the early phases.


For treatment sessions, the taping is removed, and the therapist supports the foot in the downward pointing (plantarflexed) position to prevent the broken ends of the tendon from separating whenever the patient changes position on the couch.

The patient uses crutches at first, but takes weight through the foot in the cast. The crutches are abandoned as soon as the patient feels confident enough to walk without them using the cast.
Physical treatments and self-help measures are initiated straight away, using massage to promote the circulatory flow and graded exercises to maintain activity in the muscles which are not involved in the rupture.

The phases of the recovery programme are described below.
This treatment method carries several advantages. There is minimal loss of neuromuscular function in the uninjured muscles of the leg; the physiotherapist can feel and see the state of the leg through all stages of the recovery period; therapist and patient can be aware immediately the tendon has re-united; the patient can safely do strenuous fitness exercise involving the rest of the body, starting as soon as desired after the injury; the patient can take a bath or shower (with due care!), including the injured leg, from the earliest stage; and can feel in control during the recovery process.
I first undertook this treatment programme when a close friend ruptured her Achilles tendon playing squash and told me she didn’t want either of the two standard treatments, so “you have to think of another, better way”. She recovered fully to resume squash, and later took up such esoteric pursuits as kick boxing, in between having four children.
Patients who go through this treatment method have to take full responsibility for their leg at all times. It’s not for those who like to believe that recovery depends on the surgeon’s knife or a magic pill. Nature will heal torn tissues in a healthy person. It is important to understand and believe that this is so.
Traditional conservative treatment
A plaster-of-Paris cast may be applied to the whole leg at first, and later re-made to cover just the lower leg. The patient’s foot is held turned in and pointing downwards (technically in plantarflexion and inversion) for the first period, and crutches are used to avoid taking weight through the foot. At intervals the plaster is re-applied to bring the foot gradually up towards a right angle, and the patient starts to take some weight through it. The overall period in plaster may be as long as twelve weeks, and varies according to the opinion of the surgeon or doctor in charge of the case.
The plaster cast treatment has some unavoidable disadvantages. It causes weakening of all the encased muscles, including those which are not damaged. The blood flow in the leg slows down because there is so little muscle activity, especially during the non-weightbearing phase, when the pumping impulse through the sole of the foot is also missing. It is not possible to monitor the state of the leg, except at the times when the plaster is changed. If the leg swells inside the plaster, it causes discomfort, and sometimes leads to potentially serious circulatory complications. Skin condition also changes within the plaster.
Surgery
The repair operation may be done through a scar cut through the skin,which is known as open surgery, or “blind” using the “Ma technique”, named after its inventor. After surgery, a cast is applied, usually to the lower leg only, holding the foot pointing down and inwards (in plantarflexion and inversion). The cast may surround the lower leg, otherwise it may be a front-slab, open at the back of the leg over the scar. In some cases a removable castis applied. The surgeon dictates how quickly the cast is removed and when the patient is allowed to take weight through the leg.
Infection in the scar is one of the complications which can arise following surgery. It is less likely to happen with the closed technique. Infection is usually treated with antibiotics. Most often, the problem is resolved within a few days, but if the repaired area of the tendon has been disrupted, further surgery may be needed at a later stage.
Choosing treatment
The choice of treatment may be dictated by circumstances. Because the injury is so severe and dramatic, the patient is usually treated in the casualty department, and may be asked to make a quick decision about whether to have the tendon repaired surgically. However, if the tendon is protected in the correct position in a cast or brace, you can opt for this as a temporary measure. It gives you time to work out what you want to do, and, if you wish, to seek a second opinion.
Patients with Achilles tendon rupture are often warned about the dangers of re-rupture, and statistics may be quoted to persuade the patient to choose surgery as against the traditional conservative treatment of plaster cast immobilization. In fact, whatever the treatment method used, full recovery depends on rehabilitation. In my experience, if the rehabilitation process has been properly adhered to from start to finish, the risk of re-rupture is minimized in all cases.
You must feel confident that the surgeon or practitioner is expert in dealing with Achilles tendon rupture, and you should be prepared to ask relevant questions about the options. Of the operations to repair the tendon, the closed Ma technique is preferable to surgery through a scar, if the surgeon is experienced and skilled at it. The active rehabilitation treatment is a better non-surgical option than the plaster cast. Rehabilitation care is a must in all cases.
Rehabilitation
If you have a phase in a plaster cast, post-operatively or otherwise, you should do exercises to maintain your blood flow, as well as all the uninjured muscles of your whole body. You can choose exercises from the sections "exercises explained " and "exercise machines" if you don’t know any suitable ones of your own.
First phase, keep on your toes!
In the active rehabilitation system, or after the plaster cast has been removed, the first priority for recovery is to build up strength in the calf muscles and Achilles tendon using non-weightbearing exercises, while maintaining the correct length of the tendon. This means using a protective splint with the heel raised, or wearing shoes with high heels, to prevent the heel from going down during daily life. Exercises for the whole leg are also included, to minimize the effects of limping. I always include electrical muscle stimulation for the knee’s vastus medialis obliquus muscle within the treatment sessions, to protect against secondary kneecap pain.

As soon as possible, depending on the patient’s confidence, I introduce progressive weightbearing exercises, keeping the foot in the pointed position and the knee bent at first, to prevent the tendon from lengthening out while it is still weak. The patient always stands close to a support such as a table or rail, or uses crutches.

A good way of measuring progress is to press the ball of the foot down on a weighing scale, keeping the heel up.

Once calf strength has increased enough, standing on tip-toe on both legs and shifting the weight slightly over the injured leg prepares the patient to take his or her whole weight through it. Of course, a support or crutches should be used when trying this at first.
Second phase: letting the heel down
Once the you can take full weight (or almost full weight) through the ball of the foot with the knee straight, it is time to stretch the calf musculature very gradually in order to bring the heel downwards by stages. At this point you use shoes with lower heels or less heel cushioning.
Once the foot can be placed flat on the floor comfortably, the you practise balancing on the injured leg, first on a firm surface and later perhaps on a mini-trampoline or wobble board. Exercises which involve trying to raise the heel to stand on tip-toe are introduced. This involves standing up, holding a support, and carefully raising the heels. At first, most of the weight will be held over the uninjured leg, and then gradually, over time, the you can transfer more weight over the injured leg as it strengthens and you gain confidence.
As the tendon regains its pliability, especially after open surgery or immobilization in a plaster cast, it is fairly common for the patient to experience a sudden sharp pain in it during a simple weightbearing movement. This may feel frighteningly as though the tendon has broken again but it is usually simply the result of adhesions (tightened tissue around the tendon) giving way, after which the tendon feels much more relaxed. (Don't worry, this kind of episode will not cause the tendon to lengthen unduly.)
Third phase: returning to full activity
Once you can take full weight through the injured leg and can walk and jog without limping, the exercise programme is gradually extended in easy stages to include more demanding weightbearing and dynamic exercises. The basic strengthening exercises for the calves should be maintained throughout and should remain part of your regular exercise routine indefinitely. The conclusion of the rehabilitation programme is reached when the soleus muscle is functioning efficiently, you can go up and down on the toes with the knee straight (the calf raise exercise), and can also sprint and change direction, skip, hop and jump, without limitation, fear or pain.
Recovery time
Full recovery can be expected in all cases, provided that you have followed the rehabilitation programme properly. This applies even when rehabilitation has been delayed, for instance because the initial diagnosis was missed or complications arose.
Just remember, there are no short cuts! It generally takes at least nine months to return to explosive sports safely. Progress is slower if the rehabilitation programme is not set or followed, if you are fearful of re-rupture, or if there are complications such as reflex sympathetic dystrophy. Even if you decide not to resume demanding sports such as squash, don’t use this as an excuse for failing to take on or complete the remedial exercise programme. Incomplete recovery from Achilles tendon rupture can cause secondary problems in your hips, knees or back, sometimes much later on. Regaining and preserving good body balance are the keys to avoiding unpleasant pains as tehyears go on!
Prevention
Knowing the risk factors, you can do much towards trying to prevent Achilles tendon rupture. In particular, you should take care to keep your circulation free-flowing, and be aware of warning signs, such as calf cramping. Keep your calves strong and pliable. Keep yourself fit for explosive sports involving running, jumping, twisting and turning. Try to avoid hard exercise if you are feeling especially tired, or if your legs feel at all vulnerable, weak or tight. Never sit around immediately after exercising: keep moving, keep warm, warm-down and/or have a shower. All your shoes should be chosen with care, and any with high backs should be cut down.


